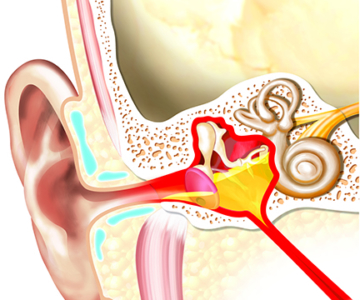
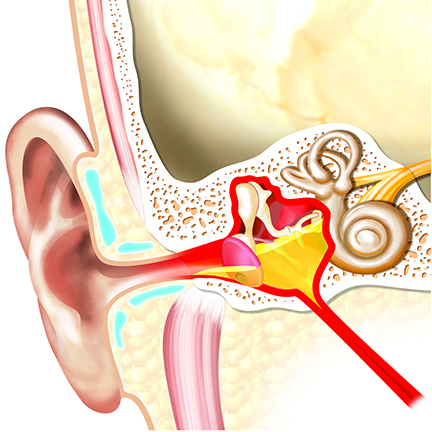
Before the first implantable Cochlear™ Baha® System was launched, one of the only solutions available to those that could not benefit from air conduction hearing aids was bone conductors fitted to steel headbands or glasses. Although it is commonly agreed that a preoperative trial is important to provide candidates with realistic expectations,1-3 similar devices are still being used for patients testing bone conduction as part of the counselling process for an implantable solution. In 2002, the Baha Softband was developed by Cochlear as a solution for children that were too young, or not ready for an implantable solution. This device has sometimes been used as a demo solution, providing a more comfortable alternative to headbands or testbands. However, the aesthetics of the Softband do not appeal to everyone. Indeed, previous research has shown that the most common reason to reject the proposal of an implantable bone conduction solution is the cosmesis.4 It could be hypothesized that the use of steel headbands and the Softband as demonstration devices have created additional barriers to the adoption of an implantable solution. Clinicians have also raised concerns that for older children that reject the Softband due to aesthetics there is no alternative solution, which in the worst case may leave them without amplification. This whitepaper summarizes the outcomes from the testing performed on the Cochlear Baha SoundArc to ensure it meets the expectations of users and their hearing care professionals.
 NCCI (National Correct Coding Initiative) edits: the purpose and impact on claims processingby Cochlear Guest Author / March 21, 2019
NCCI (National Correct Coding Initiative) edits: the purpose and impact on claims processingby Cochlear Guest Author / March 21, 2019