By Daniel M. Zeitler, MD, FACS
Cochlear Case Studies is a new series on Cochlear ProNews that highlights relevant clinical and surgical scenarios surrounding the latest hearing industry topics and research. We’re excited to partner with our professionals to highlight their experiences surrounding specific patients. The first installment will specifically feature surgeons, their cases and contributing factors for use of different electrodes.
Case study
Patient background
The patient is a middle-aged, healthy female with a non-descript learning disability referred by a community audiologist to the cochlear implant center for consideration for surgery. The patient had some degree of congenital hearing loss with no formal audiometric testing until approximately age 10, at which point a profound hearing loss in the left ear was identified, as well as a less severe hearing loss in the right ear. Bilateral hearing aids were fit, which the patient was able to use successfully for many years. Twenty years after first identification, the hearing began to progressively decline, at which point she was referred to the clinic.
The patient presented with significant right-sided tinnitus along with extensive noise exposure for many years. She had no infectious history, but reported a strong family history of hearing loss across several generations. The patient reported exploratory surgery and placement of “micro-implant” 20 years prior, along with reports of “significant anatomic abnormalities of her middle ear.” The patient was very motivated to pursue cochlear implantation and came to clinic having done significant research, then choosing the Cochlear™ Nucleus® System.
Candidate evaluation
Audiometric testing was performed and hearing aid fitting was confirmed in the binaural condition using both electroacoustic and functional gain measurements. The preoperative audiogram revealed unaided speech scores of 0% bilaterally. The decision was made to implant the right ear given the duration of profound deafness in the left ear. A non-contrasted CT of the temporal bones was performed preoperatively and both the neuroradiologist and neurotologist interpreted the right temporal bone to be normal.
Electrode selection
The Cochlear™ Nucleus® Profile™ Plus with Slim Modiolar electrode (CI632) was selected, and as with all cases in this center, a Slim Straight electrode (CI622) was ordered as backup.
Surgical observation
Intraoperatively, the mastoid anatomy was unremarkable, and the vertical facial nerve was in its usual anatomic position. Upon completing the posterior tympanotomy and entering the middle ear, there was a soft tissue mass emanating from the tympanic facial nerve and passing inferiorly over the round window niche obstructing > 90% of the round window (Figure 2).
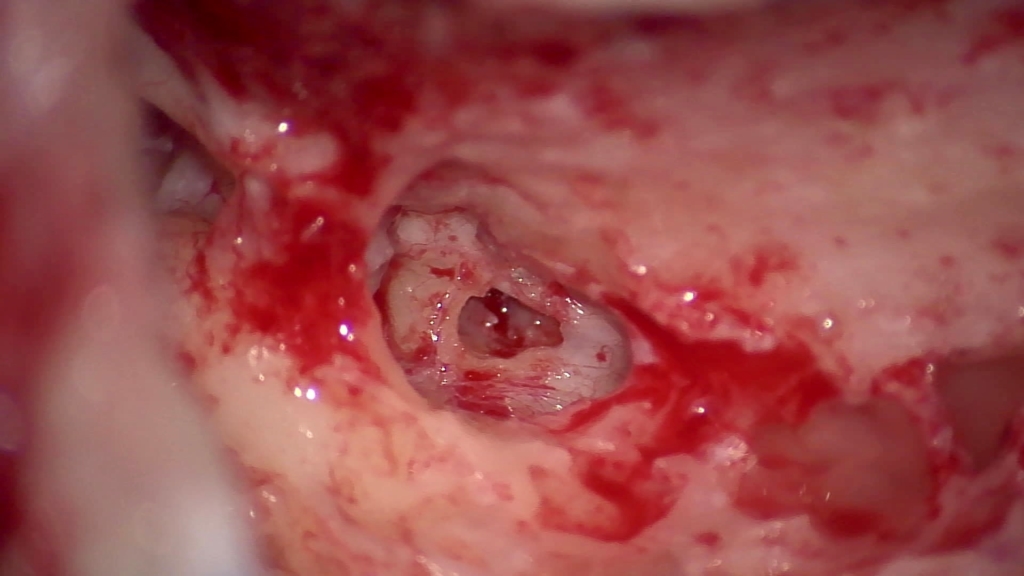
Manipulation of this mass triggered activity on the facial nerve monitor, and direct stimulation of the mass with a Prass probe at a setting of 0.3 mA produced clear and reliable activation of both the orbicularis oris and oculi muscles. Due to the inability to completely visualize nor access the round window, the surgeon determined that the silicone sheath of the CI632 would not fit in the small opening making the use of this electrode impossible. Fortunately, the CI622 had been ordered as backup, and the intraoperative decision was made to use the CI622 electrode instead due to its small diameter. A pinpoint anterior inferior opening in the round window was made with visualization of the cochlear lumen and a full, uncomplicated insertion was achieved. Intraoperative telemetry was normal along the entire array and an intraoperative skull X-ray confirmed a normal intracochlear contour of the electrode.
Postoperative re-evaluation of the temporal bone CT with specific attention to the facial nerve confirmed an aberrant branch of the facial nerve coursing over the round window that was not observed preoperatively during film study (Figure 3).
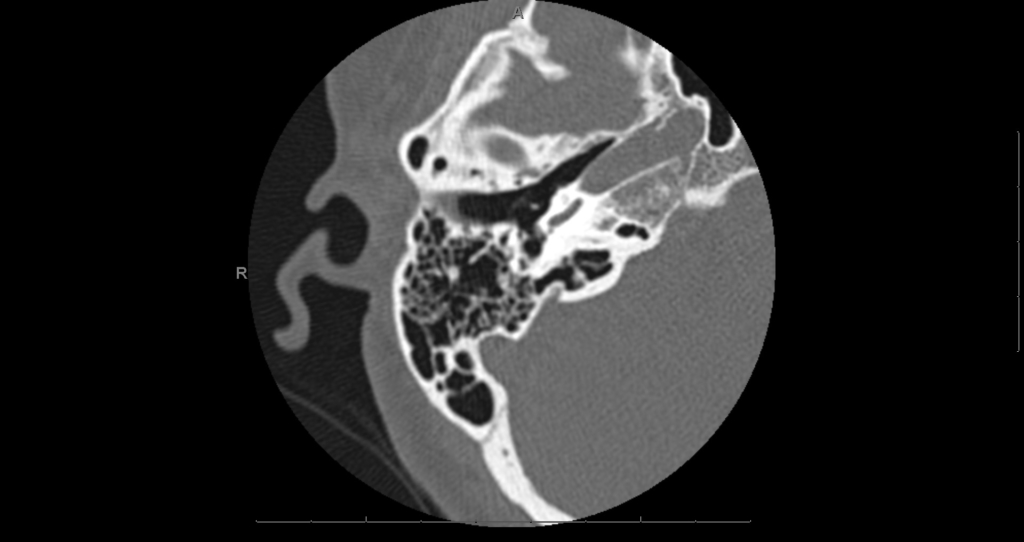
Figure 3. CT of the right temporal bone with a representative axial cut through the middle ear demonstrating a subtle soft tissue mass coursing over the round window which could be traced to the facial nerve both proximally and distally (arrow).
The patient did well postoperatively and had no facial nerve weakness or paralysis. Activation of the device was unremarkable with all 22 electrodes activated and normal loudness growth along the electrode array. Most recently, the patient returned for a follow-up and performed very well (over 85% in CNC Words).
The patient was extremely satisfied with the outcome following implantation and her quality-of-life is dramatically improved. She is now functioning incredibly well at work and is able to use both the telephone and the two-way radio. She has already requested sequential bilateral surgery on her other ear in the future.
To hear more from Dr. Zeitler, register now for the upcoming Cochlear Case Studies surgeon panel webinar on February 23rd at 5pm ET!
About the author:

Daniel M. Zeitler, MD is a board-certified Otologist/Neurotologist and Skull Base Surgeon at Virginia Mason Medical Center in Seattle, WA and Co-Director of the Listen for Life Center at Virginia Mason. Dr. Zeitler graduated magna cum laude from Northwestern University and received his MD with honors from New York University. He completed his General Surgery internship and residency in Otolaryngology/Head and Neck Surgery at New York University and his Otology, Neurotology, and Skull Base Surgery fellowship at the University of Miami Ear Institute. Dr. Zeitler currently holds the Wilske Chair for Research and the Neuroscience Institute Research Chair at Virginia Mason Medical Center. He is a Clinical Assistant Professor in the University of Washington Department of Otolaryngology and a fellow of the American College of Surgeons (FACS), the American Academy of Otolaryngology/Head and Neck Surgery (AAO-HNS), and the American Neurotology Society (ANS). Dr. Zeitler has authored over 40 peer-reviewed manuscripts and book chapters and remains active with his clinical research endeavors in the fields of cochlear implantation, single-sided deafness, and skull-based tumors.





